The Quality Jobs Quality Care Project was a three year (2013 – 2016) collaborative project between researchers from UniSA, RMIT and Flinders Universities and partners from the aged care industry. The project aim was to develop innovative workplace tools, models and benchmarks to improve job quality and the quality of services in aged care. Two groups of direct care workers were the focus of this project: personal care attendants (residential services) and community care workers (community services), being the two main occupations in the aged care workforce.
The four objectives of the Project were to:
Develop Benchmarks to evaluation interventions in workplace practices that improve both job quality and care quality.
Develop, trial and evaluate against the above Benchmarks six specific workplace interventions in three exemplary aged care organisations that improve the quality of jobs and care services.
Develop and disseminate Tools and Models that illustrate changed workplace practices that improve the quality of jobs and care services.
Collaborate with agencies, workers, care managers and care recipients through a collaborative, interactive action research methodology to develop the above Benchmarks, Interventions and Tools and Models to improve both job quality and care quality.
The Project was funded under the Australian Government: Aged Care Service Improvement and Healthy Ageing Grants Fund Priority 3a: Better Health Care Connections: Promoting better practice and partnerships - Research translation.
Three leading aged care organisations joined the project as industry partners: Brightwater (WA), HammondCare (NSW) and Helping Hand (SA). United Voice, the worker Union representing aged care workers was the fourth industry partner.
The Quality Jobs Quality Care project was implemented in four key phases.
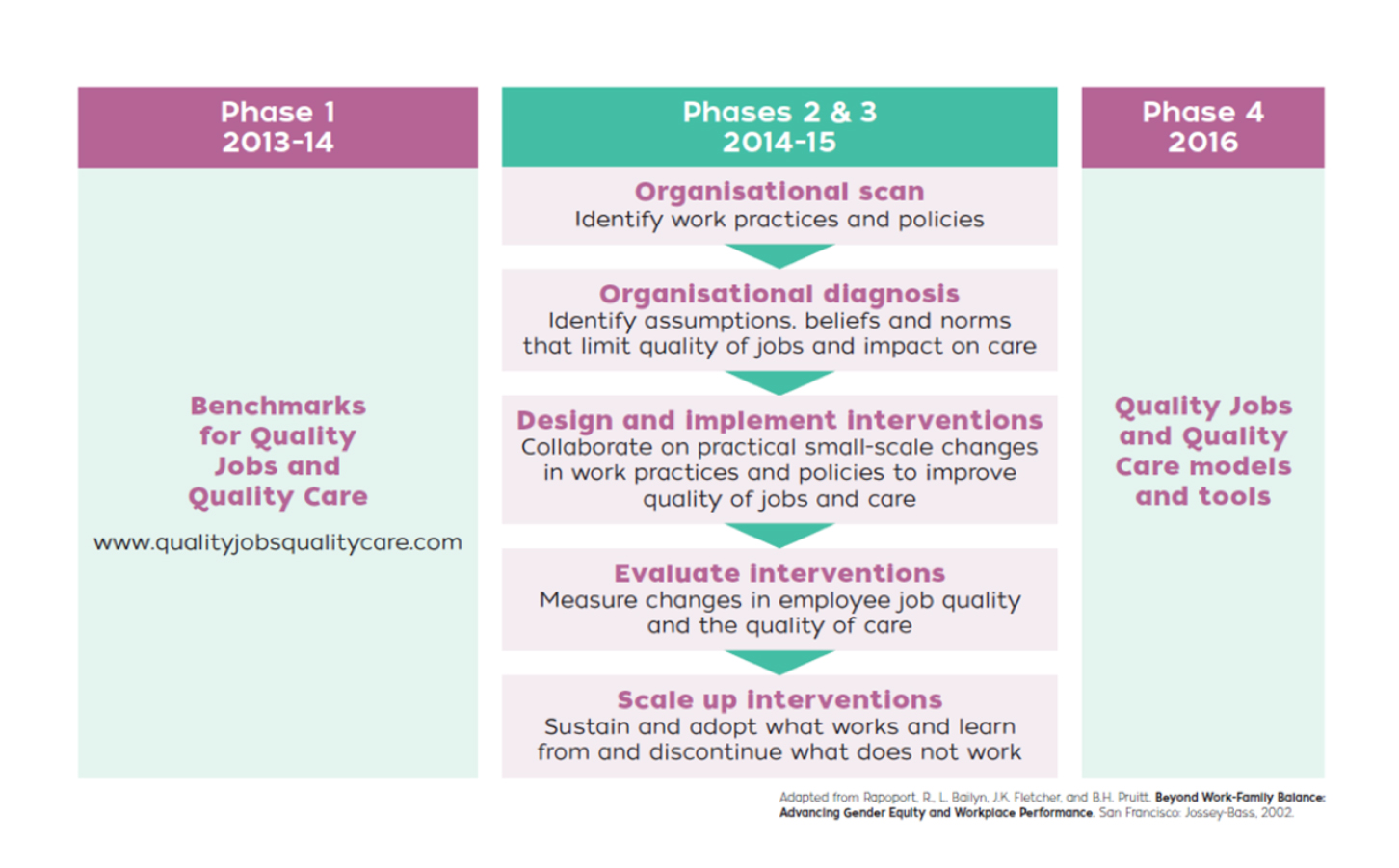
Phase 1 comprised an in-depth data analysis of the 2012 National Aged Care Workforce Census and Survey (NACWCS) (King, et al., 2013a) to identify job quality benchmarks for aged care workers (personal care attendants and community care workers). The benchmarks identified key dimensions of job quality related to employment conditions (eg work hours, level of pay), and job design (eg work demands, skill development, organisational support).
A literature review of client perspectives on quality care was also completed. Phase 1 produced three publications:
Developing Job Quality Benchmarks in Australian Aged Care Services.
Developing Job Quality Benchmarks: Work Related Injuries and Illnesses.
Client Perceptions of Quality Care in Aged Care Services.
In Phase 2, the project team engaged in close collaboration with each of the industry partners to identify which of the job quality benchmarks were a priority within their organisation. The project team conducted an organisational scan and diagnosis, including scoping interviews / focus groups with care workers, managers and supervisors, to identify priority job quality issues for the workplace interventions.
The project team worked with each partner organisation (Brightwater, HammondCare and Helping Hand) to design, implement and evaluate a workplace intervention to improve one particular aspect of job quality and to investigate associated improvements in care quality. Workplace interventions in Phase 1 involved:
Creating a specialised dementia care team to improve teamwork, working patterns and care consistency (community care workers).
Trialling a new roster system that provided regular scheduled hours to improve quality of work schedules and consistency of individualised care (community care workers).
Development of learning shifts to increase the accessibility of education and training on work time, and improve translation of skill to improved care practices (residential care workers).
Building on and integrating the insights and lessons learned from the first three interventions in Phase 2, Phase 3 involved the development and implementation of a second set of workplace interventions to improve job quality and care quality. These activities involved:
Development of a care worker mentoring program to increase support for care workers (skills, confidence, capacity) and improve quality of client care, particularly for those with complex needs (community care workers).
Trialling of a new program of wellbeing mapping to enhance multi-disciplinary team coordination and cooperation, and improve application of individualised care (residential care workers).
Consultation and scoping of a job quality intervention addressing care worker autonomy in the context of the consumer directed care environment (community care workers).
Phase 3 also included a qualitative study of key aspects of job quality for aged care workers in collaboration with United Voice, comprising interviews with Union members in NSW, SA and WA.
Phase 4 involved the translation of the knowledge, experience and insight gained in the first three project phases into a set of practical and useful tools and resources for the aged care sector. The Quality Jobs Quality Care toolkit is designed to guide and support aged care organisations to develop, implement and evaluate workplace interventions (described as ‘small scale change’ in the toolkit) to improve job and care quality. The toolkit draws on established research evidence and the knowledge and lessons learned from the project activities to present a 6-step program for small scale change (workplace intervention) to improve job and care quality that is specially tailored for aged care organisations. Key resources in the toolkit include:
Information resources providing accessible summaries of research on job quality, care quality, small scale change and evaluation.
Worksheets providing user-friendly templates to guide activities from collaboration and consultation through to evaluation and scaling up.
Case studies describing real life examples of small scale changes to improve job and care quality (the Project interventions).
Information sheets providing useful points of reflection and review on the aged care industry, care quality and the Quality Jobs Quality Care project.
Collaboration was central to the design and implementation of the Quality Jobs Quality Care Project. Central to the project were the collaborative relationships developed amongst the project team (researchers and project staff), partner representatives within the four industry partner organisations (Brightwater, HammondCare, Helping Hand and United Voice), key managers and staff within each organisation who were directly or indirectly involved in the interventions and industry stakeholders .
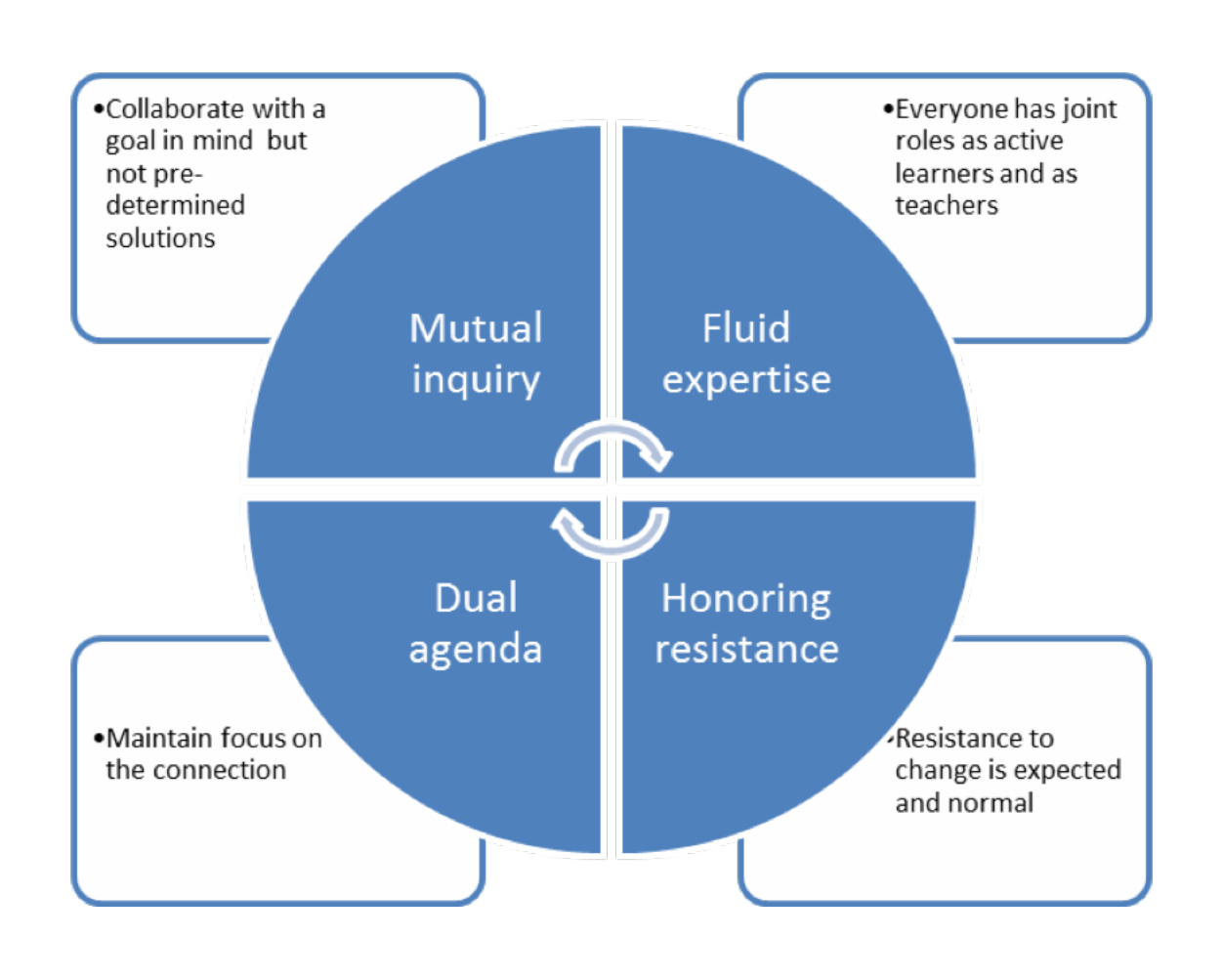
The Project adapted the Collaborative Interactive Action Research (CIAR) framework to guide the process of collaboration within the project. CIAR has been used extensively in organisational research as a collaborative, participative and practical approach to redesign work in a variety of organisational settings in the US, the UK and Australia (Bailyn, 2011; Bailyn & Fletcher, 2002, 2007; Charlesworth & Baird, 2007). It is a practical way of identifying, testing and implementing small scale changes in workplaces that meet the ‘dual agenda’ of benefitting employees and organisations. The CIAR method presumes that the organisation, its workforce and the researchers all bring expertise that can be effectively combined to produce a dynamic collaboration. The Quality Jobs Quality Care Project adapted the key principles and strategies of the CIAR approach to guide the collaboration processes within the project.
Figure 2: The four CIAR principles for effective change

Professor Sara Charlesworth
Chief Investigator
RMIT University
View Sara's university profile webpage
Sara Charlesworth is a Professor and Deputy Head of School, Research & Innovation at RMIT University’s School of Management. She is also an Adjunct Professor at the School of Management, University of South Australia. Sara’s central research interest is gender inequality in paid work and, in particular, the impact of employment and anti-discrimination regulation at the labour market, industry and workplace levels. Her research has focused on job quality, part-time work, work/life balance, sex and pregnancy discrimination and sexual harassment. She has published and presented widely in a range of academic, policy and community forums and has been actively involved in a number of key gender equality policy reviews and debates. In 2012 Sara was awarded an ARC Future Fellowship ‘Prospects for decent work and gender equality in frontline care’ and much of her recent research is focused on paid care work in Australia and internationally ( http://www.rmit.edu.au/contact/staff-contacts/academic-staff/c/charlesworth-professor-sara ).

Associate Professor Debra King
Chief Investigator
Flinders University
View Debra's university profile webpage
Debra King is a sociologist at Flinders University. Prior to a term as Dean, 2013-2016, she was a Principal Researcher at the National Institute of Labour Studies. She has expertise in qualitative research methods and survey research, with an overall interest in the meaning and experience of work and, in particular, the emotional dimensions of work. Her current research interests include working in aged care and the relationship between work and wellbeing. She has led research projects in a range of social and health care settings, and has published and presented widely on the aged care workforce. Debra has been actively involved in professional and policy settings including terms as President of The Australian Sociological Association, co-convenor of the Australian Paid Care Research Network and is a member of the Work and Family Policy Roundtable.

Dr Natalie Skinner
Senior Research Fellow
University of South Australia
Natalie Skinner is a leading expert on health and wellbeing in the workplace. She has conducted research on a range of issues including stress and burnout, job satisfaction, work overload and more recently the interaction between work and life. Much of her research has focused on the health workforce. Her background is in psychology, public health and the alcohol and other drugs field. She also has an interest in strategies to bridge the gap between research and practice to support evidence-based policy making and organisational interventions. She co-authored Time Bomb: Work, rest and play in Australia today.

Jacquie Smith
Senior Project Leader
University of South Australia
Jacquie Smith’s background is in health, she holds a professional qualification as a registered nurse, a post-graduate qualification in health service management and has policy and practice interest areas in workforce innovation and reform, aged care and public health. Her work has spanned the public and not-for-profit health sectors at both state and national level in Australia. Most recently Jacquie has led a large national workforce and innovation reform program in aged care, focused on increasing workforce productivity in community and residential care services to meet the changing health needs and preferences of older Australians.

Dr Sue Jarrad
Research Fellow
University of South Australia
Sue Jarrad's background is in aged care, including veteran’s healthcare and community aged care, and has worked for two decades at the state and national level in dementia services development, policy and advocacy. Her PhD research involved case studies on the interpretation of legal decision-making capacity in relation to older persons. She found that attitudes of paternalism and the imposition of values significantly diminished the older person’s participation in their life decisions. Sue has proposed a person-centred decision-making framework that enables others influential values to be identified, integrating the legal concepts of autonomy and capacity.
Additional team members.
Additional members of the team across the course of the project were Dr Valerie O’Keefe (Research Fellow), Dr Somayeh Parvazian (Research Assistant) and Kateryna Kalysh (Research Assistant).